Why Tax Breaks for Health Costs Backfire for Wealthy Retirees?
Analysis reveals 8 key thematic connections.
Key Findings
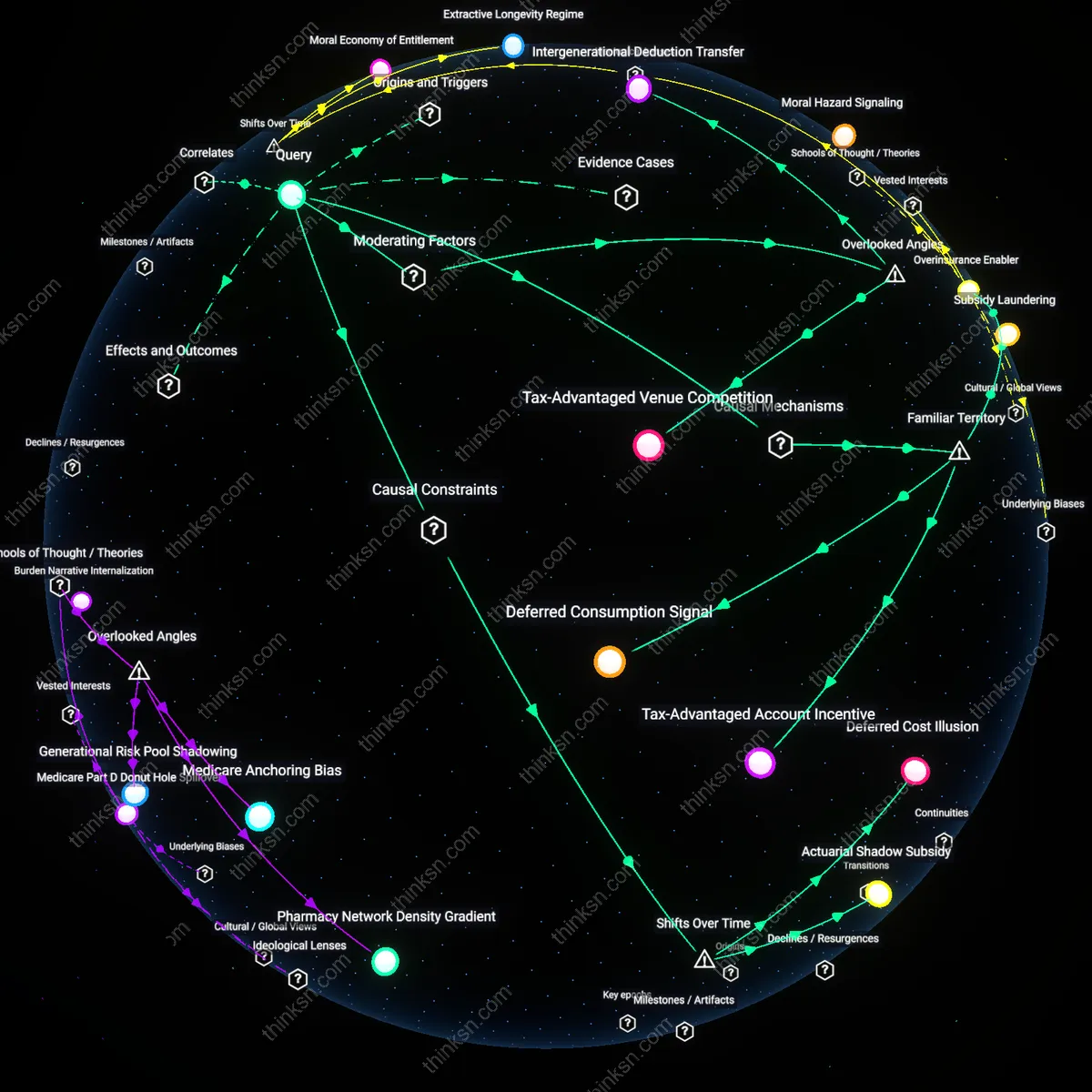
Tax-Advantaged Account Incentive
High-income individuals increase contributions to Health Savings Accounts because deductibility lowers their taxable income, which directly increases available retirement funds if earmarked for medical use. The mechanism operates through federal tax code provisions like IRS Section 223, which permits triple tax advantages—pre-tax contributions, tax-free growth, and tax-free withdrawals for qualified expenses—creating a unique fiscal incentive for high earners to treat health accounts as supplemental retirement vehicles. This is underappreciated because the public typically views HSAs purely as medical cost tools, not as stealth wealth accumulation devices enabled by structural tax asymmetries favoring affluent savers.
Deferred Consumption Signal
The tax deductibility of health savings signals to high-income households that future medical spending is pre-vetted by policy as a legitimate and rewarded form of consumption deferral, which shifts their retirement planning toward increased allocation to health-linked accounts. This works through the psychological framing of tax code endorsements—when the government subsidizes a behavior via deductions, individuals interpret it as both safe and normatively encouraged, particularly in domains like health and retirement where uncertainty is high. What's often missed is that this isn't just a financial incentive but a social cue that recalibrates expectations about what forms of saving 'count' as responsible preparation, thereby inflating health-related spending not due to medical need but to perceived fiscal legitimacy.
Overinsurance Enabler
Generous tax treatment of health expenses encourages high-income retirees to purchase more comprehensive insurance plans because the cost, when paid with pre-tax HSA or employer-premium dollars, feels artificially low, leading to overspending on coverage they would forgo if paying fully out-of-pocket. This dynamic runs through the decoupling of price perception from actual cost, where tax-subsidized payment mechanisms insulate the consumer from market signals, particularly in the Medicare Advantage and individual insurance markets where richer plans offer marginal clinical benefits at high systemic cost. The underappreciated core is that tax policy doesn’t just subsidize care—it distorts risk assessment among sophisticated savers, making them behave like overinsured consumers despite their financial literacy.
Tax-Advantaged Venue Competition
High-income individuals increasingly shift elective health procedures to out-of-state medical centers that partner with tax-advantaged retirement accounts, exploiting interstate variation in medical licensing and tax enforcement to maximize deductions not available under standard employer-sponsored plans. This behavior is driven not by medical need but by arbitrage between state-level tax policies and federal retirement account rules, a dynamic amplified when individuals anticipate retirement transitions and seek to accelerate deductible contributions to Health Savings Accounts (HSAs) or similar vehicles. Most policy analyses assume health spending under tax incentives is medically determined, but this overlooks how financial optimization incentives can drive the *geographic repositioning* of care to venues structured to capture dual tax and retirement benefits—revealing a feedback loop between retirement planning timelines and spatial patterns of medical consumption that distorts regional health spending.
Actuarial Signal Distortion
When high-income individuals structure health-care spending through tax-deferred retirement vehicles like HSAs, they inadvertently alter the risk pooling signals used by private insurers and self-insured employer plans to price future coverage. Because early, non-urgent expenditures are inflated to maximize tax deductions—such as expensive diagnostic screenings or elective imaging—the actuarial data fed into underwriting models becomes skewed toward higher utilization intensity, leading insurers to overestimate future risk and raise premiums across groups. This dynamic is rarely considered in tax policy debates, where HSA contributions are treated as neutral savings vehicles, yet it reveals that tax-incentivized spending can propagate *systemic pricing distortions* through feedback into actuarial systems, effectively socializing costs while privatizing tax gains.
Intergenerational Deduction Transfer
Affluent retirees routinely redirect tax-advantaged health funds into family-focused trusts or dependent care accounts, allowing younger relatives to use HSA balances for eligible expenses while the elder account holder retains control and tax protection. This transforms tax-advantaged health vehicles from individual retirement tools into intergenerational wealth conduits, increasing lifetime spending on health services not because of greater medical need but because the *effective cost to the beneficiary* is near zero and off-budget. The result is elevated utilization among lower-risk family members, artificially inflating aggregate health demand—a phenomenon obscured in macro analyses that assume tax preferences only affect direct retirees, but which becomes significant when dynastic wealth strategies intersect with HSA portability rules established under the Pension Protection Act of 2006.
Deferred Cost Illusion
The tax deductibility of employer-sponsored health insurance premiums since the 1950s created a fiscal incentive for high-income workers to consume more comprehensive coverage, mistaking tax-advantaged spending for personal savings. As wage controls during World War II led firms to offer health benefits as non-taxable compensation, a feedback loop emerged where rising premiums were shielded from income and payroll taxes, making expensive plans appear cheaper than they were in after-tax terms. This mechanism obscured the true cost growth from individual perception, especially among high earners with greater access to such plans, who increasingly optimized for coverage breadth over cost efficiency in retirement planning. The non-obvious insight is that the illusion of saved costs—fueled by mid-20th century tax policy—is what drives overspending decades later, not current medical prices alone.
Actuarial Shadow Subsidy
The post-1980 transition from defined-benefit pensions to defined-contribution retirement plans decoupled health planning from employer liability, pushing risk onto individuals who then over-insure in anticipation of unpredictable costs, particularly when tax incentives amplify coverage appeal. High-income earners, facing lower marginal tax rates on contributions to medical savings vehicles like FSAs and HSAs, exploit these accounts not just for savings but as forced consumption paths—since unused funds are forfeited or taxed, they spend preemptively on eligible services or devices even when marginal benefit is low. As insurance design evolved to require active consumer choice, the cognitive load of managing tax-advantaged health savings increased, and with it, the tendency to overspend near plan-year ends to avoid loss, mistaking tax efficiency for fiscal prudence. The non-obvious revelation is that the real subsidy isn’t in tax codes alone, but in the actuarial miscalibration of personal risk under a system that rewards premature or excess spending to maintain tax privilege.